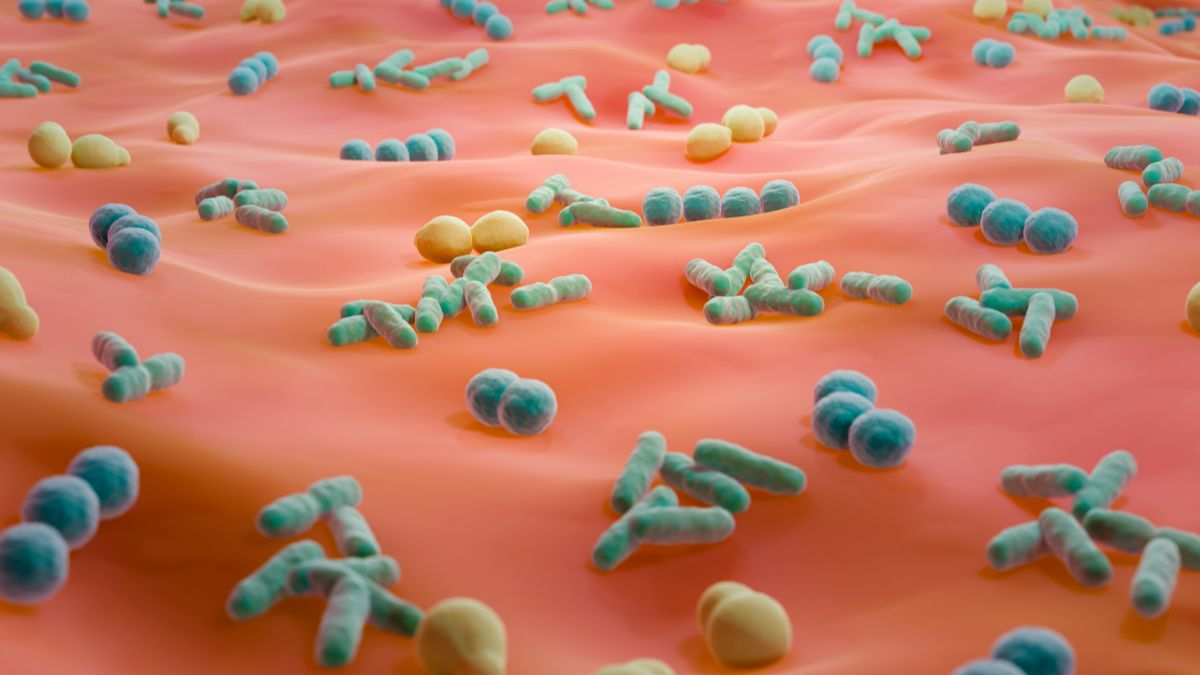
Your skin feels like a wall. It feels solid, personal, clean—something that belongs only to you. But in reality, your skin is not a silent surface. It is an ecosystem. It is a living landscape filled with microscopic life that has been growing, adapting, and thriving on human bodies for as long as humans have existed.
Right now, at this exact moment, billions of bacteria are living on you. They inhabit the ridges of your fingerprints, the folds around your nose, the damp warmth of your armpits, and the oily surface of your forehead. They cling to hair follicles and hide inside pores. Some of them are helpful, some are harmless, and some have the potential to become extremely dangerous under the right conditions.
That last part often surprises people. Many imagine that the bacteria on skin are enemies waiting to attack. But the truth is more unsettling and more fascinating: most dangerous skin bacteria are not invaders. They are residents. They are long-term tenants of your body. Many have been with you since infancy.
They don’t always cause disease. In fact, most of the time they don’t. But when the balance of your skin ecosystem is disturbed—by injury, immune weakness, medical devices, chronic skin conditions, or even antibiotic overuse—some of these familiar organisms can shift from peaceful coexistence into opportunistic violence.
The bacteria living on your skin are not monsters. They are survivors. And sometimes survival makes them dangerous.
The Skin Microbiome: A Hidden World on the Surface of Your Body
The skin microbiome refers to the community of microorganisms living on the skin. This includes bacteria, fungi, viruses, and even microscopic mites. These organisms form complex relationships with one another and with your body. They compete for space, feed on skin oils, and influence the chemistry of your skin.
Different regions of the skin support different microbial communities. Dry areas like the forearms host different bacteria than moist areas like the groin. Oily regions like the face and upper back support bacteria that thrive on sebum, the oily substance produced by sebaceous glands.
This diversity is not random. Your skin is a patchwork of environments. Temperature, moisture, pH, oxygen levels, and nutrient availability vary from one location to another, shaping which microbes can survive there.
In many ways, your skin microbiome acts like a biological security system. Beneficial bacteria occupy space and resources, preventing harmful invaders from establishing themselves. Some produce antimicrobial substances that suppress pathogens. Others help train your immune system, teaching it what to ignore and what to fight.
But this system is not perfect. It depends on balance. When that balance breaks, the same bacteria that normally protect you can become dangerous.
What Makes a Skin Bacterium “Dangerous”?
The phrase “dangerous bacteria” often brings to mind rare infections or exotic diseases. But dangerous bacteria on your skin are usually common species that become harmful only in specific situations.
A bacterium becomes dangerous when it has the ability to invade tissue, evade immune defenses, or produce toxins that damage cells. Some bacteria have enzymes that break down skin barriers. Others form biofilms—protective layers that allow them to cling to surfaces and resist antibiotics. Some can enter the bloodstream and spread to organs, causing systemic infection.
Danger is also influenced by the host. A healthy person with intact skin may carry potentially harmful bacteria without ever becoming sick. But someone with eczema, diabetes, a surgical wound, or a weakened immune system may be vulnerable.
This is the unsettling truth: the most dangerous bacteria on your skin are often dangerous not because they are rare, but because they are always nearby.
Staphylococcus aureus: The King of Skin Threats
If there is one bacterium that deserves the title of “most dangerous skin resident,” it is Staphylococcus aureus.
Staphylococcus aureus, often called “staph,” is a bacterium that can live harmlessly on the skin or inside the nose of many healthy people. It is incredibly common. In fact, a significant portion of the human population carries it at any given time without symptoms.
But Staphylococcus aureus is also one of the leading causes of serious skin and soft tissue infections worldwide. It can cause boils, abscesses, impetigo, and cellulitis. It can infect cuts and surgical wounds. If it penetrates deeper into the body, it can lead to pneumonia, bone infections, heart valve infections, and bloodstream infections known as sepsis.
What makes it particularly dangerous is its arsenal of virulence factors. Staphylococcus aureus can produce toxins that destroy tissue, disrupt immune cells, and cause inflammation. Some strains produce exfoliative toxins that lead to severe skin peeling. Others produce toxic shock syndrome toxin, which can trigger a rapid, life-threatening immune reaction.
The real nightmare is that Staphylococcus aureus has also evolved resistance to many antibiotics.
MRSA: When Staph Learns to Defeat Medicine
Methicillin-resistant Staphylococcus aureus, or MRSA, is not a separate species. It is a strain of Staphylococcus aureus that has developed resistance to methicillin and related antibiotics. MRSA has become one of the most feared pathogens in hospitals and healthcare settings, but it also exists outside hospitals in the community.
MRSA is dangerous because it turns routine infections into medical emergencies. A small cut or shaving nick can become infected and develop into a painful abscess. If MRSA spreads into the bloodstream, it can become deadly.
Hospitals are particularly vulnerable because patients often have weakened immune systems, open wounds, or medical devices like catheters. MRSA can survive on surfaces and spread through contact, making it difficult to control.
Community-associated MRSA can spread in crowded settings such as gyms, dormitories, prisons, and sports teams. Skin-to-skin contact and shared towels or equipment can help it spread quickly.
The presence of MRSA on skin does not mean you are sick, but it does mean the bacterium has access to you at all times. If your skin barrier breaks, it may seize the opportunity.
Staphylococcus epidermidis: A Friendly Neighbor With a Dark Side
Staphylococcus epidermidis is one of the most common bacteria found on human skin. Unlike Staphylococcus aureus, it is usually considered beneficial. It helps prevent harmful bacteria from colonizing by occupying space and competing for nutrients.
But Staphylococcus epidermidis has a darker side. It is an opportunistic pathogen, especially dangerous in hospital environments. Its greatest weapon is its ability to form biofilms.
A biofilm is a slimy protective layer made of bacterial cells and extracellular material. Inside a biofilm, bacteria become much harder to kill. Antibiotics may not penetrate effectively, and immune cells struggle to attack them.
Staphylococcus epidermidis is notorious for colonizing medical implants such as artificial joints, heart valves, pacemakers, and intravenous catheters. Once established, it can cause chronic infections that are difficult to treat and sometimes require removal of the device.
In everyday life, it rarely causes serious problems. But in modern medicine, where devices are inserted into the body, Staphylococcus epidermidis can transform from harmless resident into persistent enemy.
It is a reminder that danger is not always about aggression. Sometimes danger comes from patience and persistence.
Cutibacterium acnes: The Acne Bacterium That Can Become a Threat
Cutibacterium acnes, formerly known as Propionibacterium acnes, is best known for its role in acne. It thrives in oily regions of the skin, particularly inside hair follicles and pores where oxygen is limited.
For many people, Cutibacterium acnes is simply part of normal skin biology. It breaks down sebum and contributes to the skin’s chemical environment. But under certain conditions, it can trigger inflammation. When follicles become clogged, Cutibacterium acnes can multiply, stimulating immune responses that lead to redness, swelling, and pus formation.
Acne itself is not usually dangerous in the life-threatening sense, but it can cause scarring, psychological distress, and chronic skin inflammation. In severe cases, acne can become cystic and deeply painful.
Beyond acne, Cutibacterium acnes can occasionally cause serious infections, particularly involving implanted devices. It has been associated with infections in artificial joints, heart valves, and even post-surgical wounds. These infections are often slow-growing and may go unnoticed for a long time.
Cutibacterium acnes is an example of how a bacterium can be both normal and troublesome, depending on where it is and what conditions allow it to flourish.
Streptococcus pyogenes: The Flesh-Eating Possibility
Streptococcus pyogenes is not always present on the skin, but it can colonize it and is one of the most dangerous bacteria associated with skin infections.
This organism, also known as Group A Streptococcus, is famous for causing strep throat. But it can also cause skin infections like impetigo and cellulitis. In severe cases, it can lead to necrotizing fasciitis, often sensationalized as “flesh-eating disease.”
Necrotizing fasciitis is rare, but it is terrifying. The bacteria spread rapidly along the connective tissue beneath the skin, releasing toxins that destroy tissue and disrupt blood supply. Without immediate treatment—often involving emergency surgery and antibiotics—the infection can be fatal.
Streptococcus pyogenes can also cause streptococcal toxic shock syndrome, where bacterial toxins trigger a massive immune response leading to organ failure.
The frightening part is that Streptococcus pyogenes does not always require a large wound. Sometimes it enters through a minor cut or insect bite.
It is not a constant resident for everyone, but when it is present, it is one of the most dangerous bacteria that can be involved in skin infections.
Corynebacterium: The Odor-Makers With Opportunistic Potential
Corynebacterium species are common on human skin, especially in moist areas such as the armpits and groin. They are famous not because they cause frequent disease, but because they contribute to body odor.
Sweat itself is mostly odorless. The smell develops when bacteria metabolize sweat compounds and release volatile chemicals. Corynebacterium is one of the key players in this process.
Most Corynebacterium species on the skin are harmless, but some can cause infections in vulnerable individuals. Certain strains can infect wounds or cause opportunistic infections in people with weakened immune systems.
The more famous relative of this group is Corynebacterium diphtheriae, the bacterium that causes diphtheria. However, diphtheria is primarily a respiratory infection and is now rare in vaccinated populations. Skin colonization and cutaneous diphtheria can still occur in some areas, but it is not a common threat in everyday life for most people.
Corynebacterium illustrates a broader truth: even bacteria associated with something as ordinary as body odor can become harmful in the wrong context.
Pseudomonas aeruginosa: The Wet-Environment Predator
Pseudomonas aeruginosa is not always considered a normal skin bacterium, but it can colonize skin, especially in moist environments. It is notorious in hospitals and among people with burns, chronic wounds, or weakened immune systems.
This bacterium thrives in water and damp places. It can live in sinks, pools, hot tubs, and even poorly cleaned medical equipment. On the skin, it is often associated with infections that develop in wet conditions.
One common example is “hot tub folliculitis,” where Pseudomonas infects hair follicles after exposure to contaminated water. The result is an itchy rash of inflamed bumps.
In more serious cases, Pseudomonas aeruginosa can infect wounds, burns, and surgical sites. It can also cause life-threatening infections in hospitalized patients, especially those on ventilators or with catheters.
Pseudomonas is dangerous because it is naturally resistant to many antibiotics and can quickly develop further resistance. It also produces toxins and pigments that can damage tissue.
In the wrong environment, it is one of the most aggressive bacteria a human can encounter.
Acinetobacter baumannii: The Hospital Survivor
Acinetobacter baumannii has become infamous as a hospital-acquired pathogen. It can survive on skin and on surfaces for long periods, making it exceptionally difficult to eliminate in healthcare settings.
This bacterium is particularly dangerous because it often infects patients with severe injuries, ventilator support, or compromised immune systems. It can cause pneumonia, wound infections, and bloodstream infections.
Acinetobacter baumannii is sometimes called a “superbug” because many strains are resistant to multiple antibiotics, including some of the strongest ones available. Treatment options can be limited, and outbreaks can be difficult to control.
For healthy people in everyday life, Acinetobacter is not typically a major threat. But its ability to persist, spread, and resist treatment makes it one of the most feared bacteria that can be found on skin in certain environments.
Its danger lies in its resilience. It does not need to be the most aggressive predator if it can outlast every attempt to destroy it.
Enterococcus: A Gut Bacterium That Can Colonize Skin
Enterococcus species, particularly Enterococcus faecalis and Enterococcus faecium, are normally found in the intestines. However, they can colonize skin, especially in hospital settings or in people with wounds.
Enterococcus is an opportunistic pathogen. It can cause urinary tract infections, wound infections, and bloodstream infections. It is particularly concerning because some strains have developed resistance to vancomycin, a powerful antibiotic used as a last resort. These strains are known as VRE, or vancomycin-resistant Enterococcus.
When Enterococcus becomes established in a hospital environment, it can spread through contact and become a serious infection control challenge. It is not the most common skin resident, but it can become part of the skin microbiota under certain conditions.
Enterococcus is dangerous because it blurs the boundary between internal and external ecosystems. It is a reminder that bacteria do not respect the categories humans assign them. Skin, gut, mouth, and environment are all connected through contact and movement.
Why Your Skin Usually Keeps You Safe
If all these dangerous bacteria exist on skin, why aren’t we constantly infected?
The answer is that healthy skin is one of the most powerful defensive structures in nature. It is not just a physical barrier. It is an active immune organ.
The outermost layer of skin, the stratum corneum, is made of dead cells packed tightly together, forming a tough shield. Skin is slightly acidic, which discourages many harmful bacteria. It produces antimicrobial peptides that can kill microbes. Sweat contains salt and other compounds that create harsh living conditions for many organisms.
Your immune system also constantly monitors the skin. Immune cells patrol for signs of invasion. When bacteria breach the barrier, inflammation is triggered quickly to contain the threat.
Even the beneficial bacteria help. They occupy space, consume resources, and prevent pathogens from gaining a foothold. In many cases, your microbiome is part of your immune defense.
Most of the time, the bacteria on your skin are not your enemies. They are part of your biological identity.
When Skin Bacteria Become Dangerous
The danger arises when bacteria gain access to deeper tissue. This usually happens through damage or disruption of the skin barrier.
A cut, scrape, burn, surgical incision, insect bite, or shaving nick can become an entry point. Skin conditions like eczema can create microscopic cracks that allow bacteria to penetrate. Chronic illnesses like diabetes can reduce circulation and impair healing, making infection more likely.
Medical devices can also create opportunities. Catheters, implants, and tubes bypass the skin’s natural defenses and provide surfaces where bacteria can form biofilms.
Antibiotic use can disrupt the normal microbiome, killing beneficial bacteria and allowing resistant strains to dominate. Harsh overuse of antibacterial soaps and frequent chemical exposure can also alter the skin environment, potentially making it easier for harmful organisms to thrive.
Even stress and hormonal changes can influence the skin microbiome by altering sweat production, oil levels, and immune responses.
Infection is not always about exposure to new bacteria. Often, it is about changing conditions that allow familiar bacteria to behave differently.
The Most Dangerous Threat Is Antibiotic Resistance
Perhaps the most frightening aspect of dangerous skin bacteria today is not their presence, but their evolution.
Bacteria reproduce rapidly. They mutate. They exchange genetic material. In environments where antibiotics are frequently used, bacteria with resistance genes survive and multiply. Over time, strains that once would have been easily treated become nearly untouchable.
This is why MRSA, VRE, and drug-resistant Pseudomonas and Acinetobacter are such major medical concerns. These bacteria do not need to be more aggressive than others. They only need to be harder to kill.
Antibiotic resistance turns ordinary infections into potentially lethal ones. It increases hospital stays, medical costs, and mortality rates. It threatens the effectiveness of surgeries and cancer treatments, which depend on infection control.
In the future, the most dangerous skin bacteria may not be the ones that produce the deadliest toxins, but the ones that modern medicine can no longer reliably defeat.
How to Live With Skin Bacteria Without Fear
The goal is not to sterilize your skin. That would be impossible and unhealthy. A diverse, balanced skin microbiome is a sign of normal biological function.
Good hygiene matters, but hygiene is not the same as constant disinfection. Washing hands regularly, keeping wounds clean, and avoiding unnecessary antibiotic use are far more effective strategies than trying to eliminate all microbes.
Skin bacteria become dangerous primarily when they enter places they do not belong. That means the best protection is maintaining the integrity of your skin barrier and being attentive to infections.
If a wound becomes increasingly red, swollen, warm, painful, or begins producing pus, it may be infected. Fever, spreading redness, or rapid worsening are warning signs that require medical attention. Some infections progress quickly, and early treatment can prevent serious outcomes.
Living with bacteria is not optional. You cannot remove them without removing yourself from the natural world. But you can understand them, respect them, and reduce the chances that they will turn against you.
The Strange Truth: Your Skin Is a Battlefield and a Partnership
It is easy to think of bacteria as villains. Many are capable of causing disease, and some can kill. But the relationship between humans and microbes is not purely hostile.
Your skin bacteria are not just threats. They are also defenders. They compete with pathogens. They influence your immune system. They help maintain the chemical environment of your skin. Without them, your skin would be more vulnerable, not less.
The most dangerous bacteria living on your skin right now are not necessarily the ones actively harming you. They are the ones quietly waiting for opportunity. They are the organisms that can transform from harmless companions into serious threats when conditions change.
Staphylococcus aureus, especially MRSA strains, stands as the most significant danger because it is common, adaptable, and capable of causing severe disease. Streptococcus pyogenes is one of the most frightening because of its potential for rapid, tissue-destroying infections. Pseudomonas aeruginosa and Acinetobacter baumannii represent the threat of antibiotic resistance and hospital survival. Even bacteria like Staphylococcus epidermidis and Cutibacterium acnes show that harmlessness is not permanent—it depends on location and circumstance.
The skin is not simply a protective layer. It is a living interface between your body and the outside world. It is where your biology meets the universe.
And on that surface, life is constantly negotiating, competing, cooperating, and evolving.
A Final Thought: The Danger Is Real, But So Is the Balance
If you could see the microbial life on your skin, you might never feel clean again. But you would also witness something extraordinary: a thriving ecosystem that has evolved alongside you, shaped by millions of years of survival.
The bacteria on your skin are ancient, intelligent in their own way, and astonishingly resilient. Some can be deadly. Most are harmless. Many are helpful.
The danger is not that they exist. The danger is forgetting that you are part of the same biological world they are.
Your skin is alive with microscopic companions, and every day your immune system keeps the peace. Most of the time, you will never notice this quiet war and quiet partnership happening on your body.
But the next time you wash your hands, treat a wound, or feel the sting of a cut, remember this: the most dangerous bacteria are not always “out there.”
Some of them are already with you.
They are waiting, not out of malice, but because nature does not choose sides. It only rewards survival.
And survival, in the microbial world, can sometimes look like danger.