Pain is one of the most universal human experiences, yet one of the least understood. It can be sharp or dull, fleeting or chronic, but in every case, it demands attention. For centuries, people have searched for ways to tame it—sometimes with herbs and rituals, and in modern times, with powerful drugs like opioids.
But opioids, for all their effectiveness, carry a heavy price: addiction, overdose, and devastating side effects. Scientists have long been searching for alternatives that could soothe pain without such risks. Now, researchers at the University of Sydney may have brought us a step closer to that future.
In a groundbreaking study published in Science, scientists have revealed a map-like system in the brainstem that controls pain differently depending on where it occurs in the body. The discovery could transform how we understand pain—and how we treat it.
The Brainstem: Highway of Survival
To grasp the significance of this finding, we need to understand the brainstem itself. Often overlooked in conversations about the brain, the brainstem is one of the oldest and most vital parts of our nervous system.
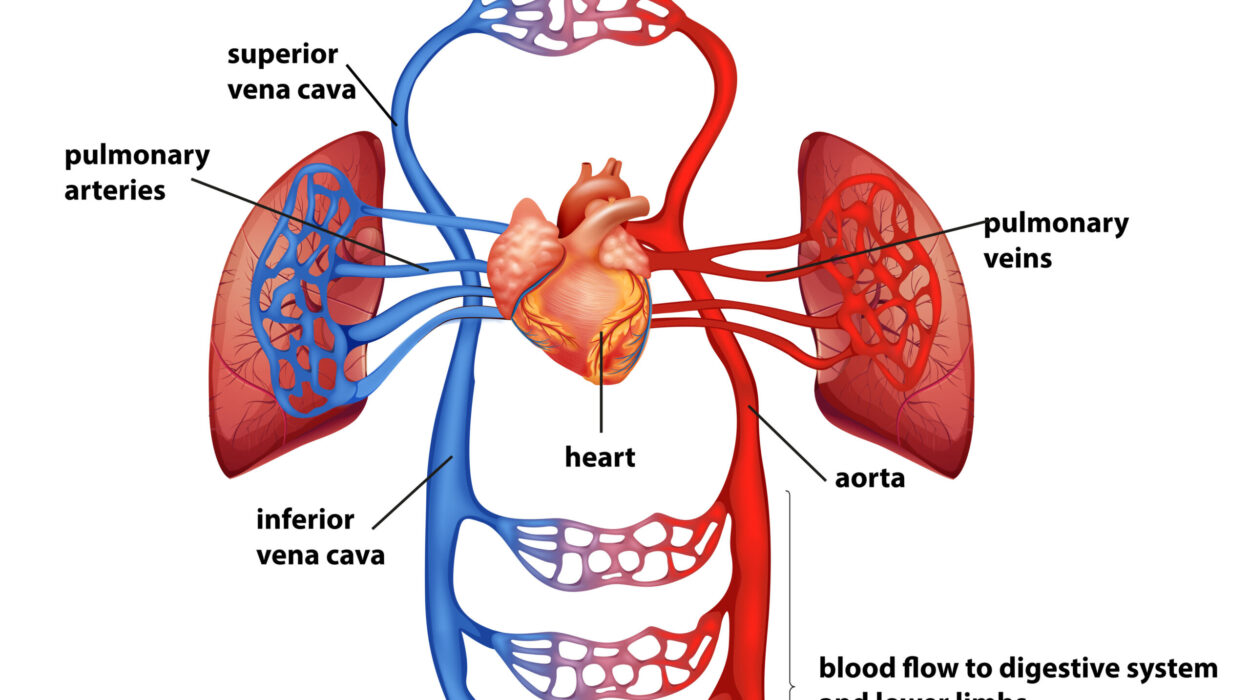
Like a highway, it connects the brain to the spinal cord, managing all signals that travel between them. It regulates the basics that keep us alive—breathing, heartbeat, alertness. And critically, it produces and releases nearly all the neurochemicals that allow us to think, feel, and survive.
Now, scientists have shown that hidden within this ancient structure lies a precise and dynamic system for controlling pain, fine-tuned to different regions of the body.
The Placebo Puzzle
The researchers unlocked this secret using something both simple and astonishing: the placebo effect.
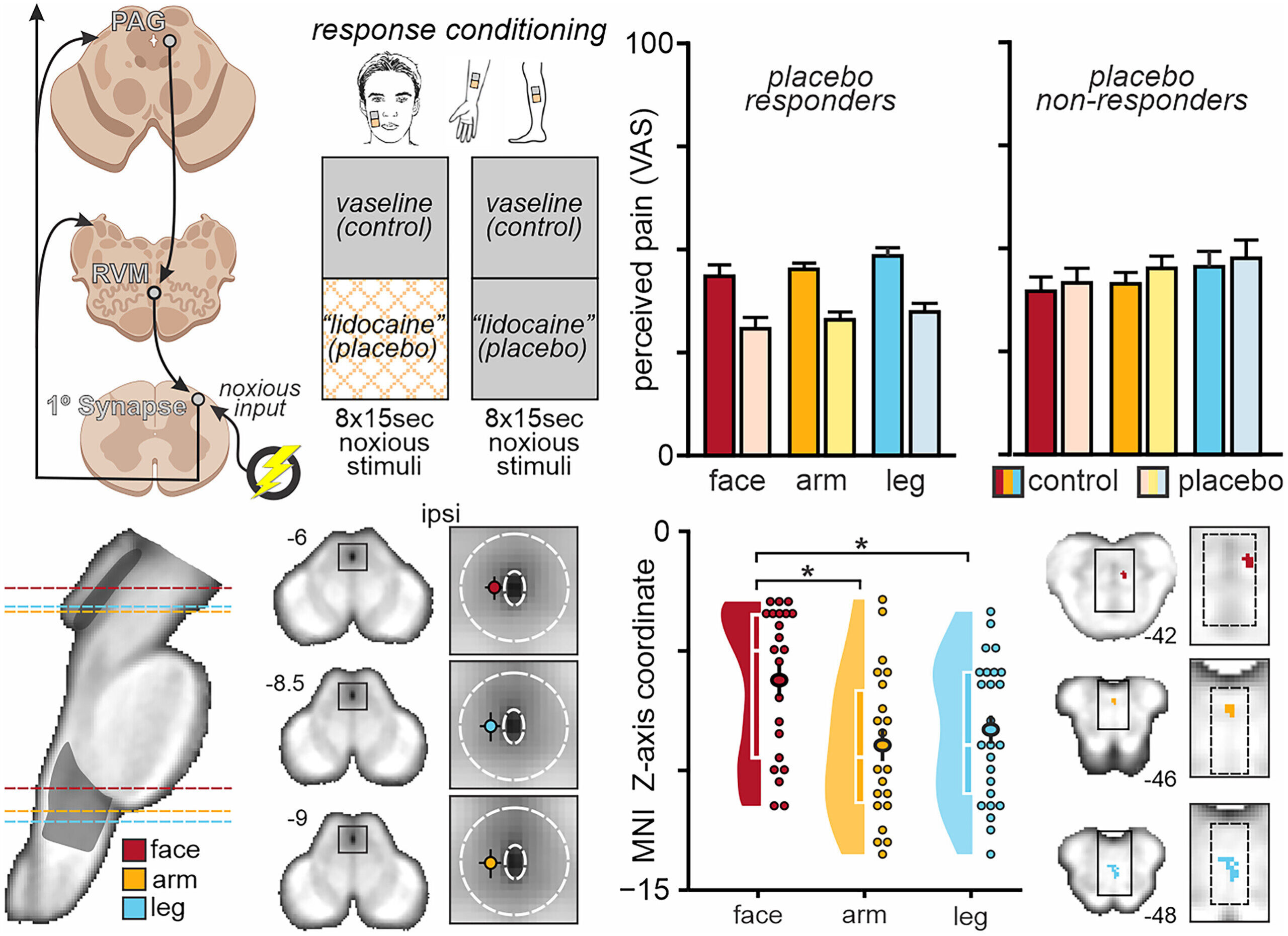
In their experiment, 93 healthy volunteers were exposed to carefully calibrated heat pain on different parts of their bodies. For some of these areas, researchers applied what participants believed was a pain-relief cream. In reality, it was a placebo. To make the illusion convincing, the scientists secretly lowered the heat temperature during conditioning, training participants’ brains to associate the cream with relief.
Later, when the same painful stimulus was applied again, many participants continued to report less pain where the cream had been applied—even though the temperature was the same. In fact, up to 61% of them experienced genuine pain relief, a textbook example of the placebo response.
This allowed the team to peer into the brain’s own pharmacy, watching how belief alone could trigger real changes in pain perception.
A Brainstem Blueprint
What they found was extraordinary. Using one of the world’s most powerful imaging tools—a 7-Tesla functional MRI scanner—the researchers were able to visualize the brainstem with unprecedented clarity.
They discovered that pain relief in the brain is not uniform. Instead, it is mapped according to body regions.
When participants experienced facial pain relief, upper areas of two key brainstem regions—the periaqueductal gray (PAG) and the rostral ventromedial medulla (RVM)—lit up with activity. But when the pain relief occurred in the arms or legs, lower parts of these same structures became active.
In other words, the brainstem tailors its response, directing pain relief with astonishing precision depending on where the pain originates. As lead author Dr. Lewis Crawford explained, “This is the first time we’ve seen such a precise and detailed pain map in the human brainstem, showing us that it tailors pain relief to the specific part of the body that’s experiencing it.”
Beyond Opioids: A Different Circuit
Perhaps the most exciting aspect of this discovery is what it suggests about alternatives to opioids. Traditionally, scientists believed placebo pain relief worked by tapping into the brain’s opioid system—a mechanism that, like morphine, dulls pain across the body.
But this study paints a different picture. The researchers found evidence that a distinct brainstem region, the lateral PAG, may be responsible for placebo-based pain relief—and it appears to operate without opioids. Instead, it may rely on cannabinoids, the same family of chemicals found in cannabis but also naturally produced by the human body.
This cannabinoid-linked pathway appears more selective, activating only in the specific regions where pain is expected to be relieved. That means therapies targeting this system could, in theory, provide highly localized pain relief without the risks and side effects of opioids.
As Dr. Crawford noted, “Opioid-based pain relief typically activates central areas of the brain and can affect the whole body, whereas the cannabinoid circuit that we identified appears to operate in more targeted regions of the brainstem.”
Hope for Chronic Pain
The implications are profound. Chronic pain affects millions worldwide, often trapping people in cycles of discomfort, disability, and dependency on powerful drugs. If scientists can learn to activate or enhance the brain’s natural, spatially organized pain relief circuits, they may one day offer therapies that are both safer and more effective.
Professor Luke Henderson, senior author of the study, put it simply: “We now have a blueprint for how the brain controls pain in a spatially organized way. This could help us design more effective and personalized treatments, especially for people with chronic pain in a specific area of their body.”
Imagine treatments that quiet pain only in the shoulder, or the lower back, or the face—without numbing the rest of the body, and without the fog of opioids. This research suggests such a future may be possible.
Pain, Belief, and the Human Brain
At the heart of this study lies a paradox: a fake cream, paired with belief, revealed one of the brain’s deepest secrets. This is a reminder that pain is never just a physical signal. It is an experience shaped by biology, psychology, and context. The placebo effect, far from being “just in your head,” is proof that belief can trigger real chemical changes in the brain.
For decades, science has treated the placebo response as a nuisance to be controlled in experiments. Now, it is becoming clear that it may hold keys to new therapies. What once seemed like a trick of the mind is, in truth, a window into the brain’s own healing systems.
The Road Ahead
The University of Sydney team’s discovery is not a cure for chronic pain—at least, not yet. But it is a map, literally and figuratively. By charting how the brainstem organizes pain relief, scientists can now explore new strategies to unlock these pathways.
Future research will need to confirm how cannabinoid circuits operate, whether they can be safely targeted, and how this knowledge can translate into real-world therapies. But the foundation has been laid.
And beyond the technical details, there is something deeply human about this story. It shows us that our brains already contain remarkable tools for relief. It shows us that belief and biology are intertwined in ways we are only beginning to understand. And it offers hope that, one day, pain may no longer have the power to dominate so many lives.
More information: Lewis S. Crawford et al, Somatotopic organization of brainstem analgesic circuitry, Science (2025). DOI: 10.1126/science.adu8846